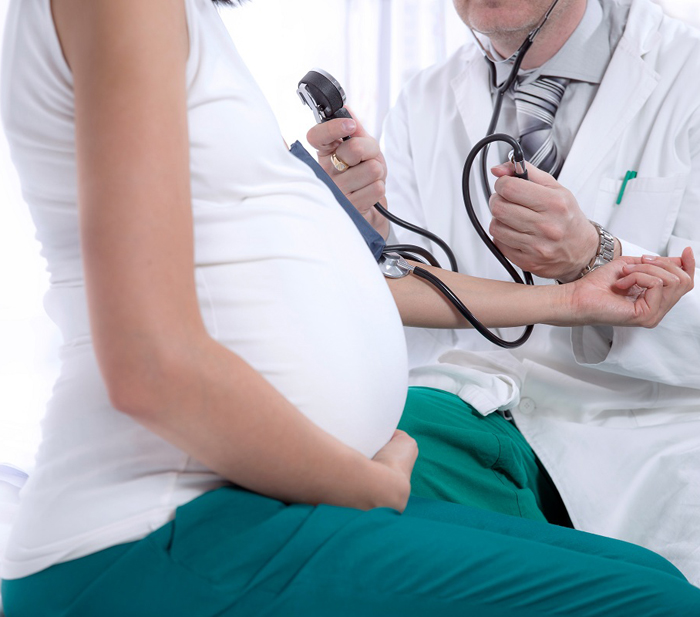
Many of my female friends became pregnant with their first child in their late 30s or early 40s, which increased their risk of common complications such as high blood pressure, gestational diabetes and preeclampsia.
Affecting over 8 million women worldwide, preeclampsia can lead to serious, even fatal, complications for both the mother and baby. The clinical symptoms of preeclampsia typically start at 20 weeks of pregnancy and include high blood pressure and signs of kidney or liver damage.
“Once these clinical symptoms appear, irreparable harm to the mother or the fetus may have already occurred,” said Stanford immunologist Brice Gaudilliere, MD, PhD. “The only available diagnostic blood test for preeclampsia is a proteomic test that measures a ratio of two proteins. While this test is good at ruling out preeclampsia once clinical symptoms have occurred, it has a poor positive predictive value.”
Now, Stanford researchers are working to develop a diagnostic blood test that can accurately predict preeclampsia prior to the onset of clinical symptoms.
A new study conducted at Stanford was led by senior authors Gaudilliere, statistical innovator Nima Aghaeepour, PhD, and clinical trial specialist Martin Angst, MD, and co-first authors and postdoctoral fellows Xiaoyuan Han, PhD, and Sajjad Ghaemi, PhD. Their results were recently published in Frontiers in Immunology.
They analyzed blood samples from 11 women who developed preeclampsia and 12 women with normal blood pressure during pregnancy. These samples were obtained at two timepoints, allowing the scientists to measure how immune cells behaved over time during pregnancy.
“Unlike prior studies that typically assessed just a few select immune cell types in the blood at a single timepoint during pregnancy, our study focused on immune cell dynamics,” Gaudilliere explained. “We utilized a powerful method called mass cytometry, which measured the distribution and functional behavior of virtually all immune cell types present in the blood samples.”
The team identified a set of eight immune cell responses that accurately predicted which of the women would develop preeclampsia — typically 13 weeks before clinical diagnosis.
At the top of their list was a signaling protein called STAT5. They observed higher activity of STAT5 in CD4+ T-cells, which help regulate the immune system, at the beginning of pregnancy for all but one patient who developed preeclampsia.
“Pregnancy is an amazing immunological phenomenon where the mother’s immune system ‘tolerates’ the fetus, a foreign entity, for nine months,” said Angst. “Our findings are consistent with past studies that found preeclampsia to be associated with increased inflammation and decreased immune tolerance towards the fetus.”
Although their results are encouraging, more research is needed before translating them to the clinic.
The authors explained that mass cytometry is a great tool to find the “needle in the haystack.” It allowed them to survey the entire immune system and identify the key elements that could predict preeclampsia, but it is an exploratory platform not suitable for the clinic, they said.
“Now that we have identified the elements of a diagnostic immunoassay, we can use conventional instruments such as those used in the clinic to measure them in a patient’s blood sample.” Aghaeepour said.
First though, the team needs to validate their findings in a large, multi-center study. They are also using machine learning to develop a “multiomics” model that integrates these mass cytometry measurements with other biological analysis approaches. And they are investigating how to objectively define different subtypes of preeclampsia.
Their goal is to accurately diagnose preeclampsia before the onset of clinical symptoms.
“Diagnosing preeclampsia early would help ensure that patients at highest risk have access to health care facilities, are evaluated more frequently by obstetricians specialized in high-risk pregnancies and receive treatment,” said Gaudilliere.
Women with preeclampsia can receive care through the obstetric clinic at Lucile Packard Children’s Hospital Stanford.
Photo by Pilirodriquez
This is a reposting of my Scope blog story, courtesy of Stanford School of Medicine.