In a new series, “Behind the Scenes,” we’re inviting Stanford Medicine physicians, nurses, researchers and staff to share a glimpse of their day.
As a science writer, I talk to a lot of health care providers about their work. But I’ve often wondered what it is really like to be a surgeon. So I was excited to speak with pediatric surgeon Stephanie Chao, MD, about her day.
Chao is a pediatric general surgeon, an assistant professor of surgery and the trauma medical director for Stanford Children’s Health. In addition to performing surgeries on children of all ages, she has a range of research interests, including how to reduce gun-related deaths in children and the hospital cost associated with pediatric firearm injuries.
Morning routine
On days that I operate, I get up between 5:50 and 6 a.m., depending on whether I hit the snooze button. I typically don’t eat breakfast. I don’t drink coffee because I don’t want to get a tremor. I’m out the door by 6:30 a.m. and at the hospital by 7 a.m. I usually go by the bedside of the first patient I’m going to operate on to say hi. The patient is in the operating room by 7:30 a.m. and my cases start.
On non-surgical days, it’s more chaotic. I have a 3-year-old and 1-year-old. So every day there’s a jigsaw puzzle as to whether my husband or I stay to get the kids ready for preschool, and who comes home early.

In the operating room
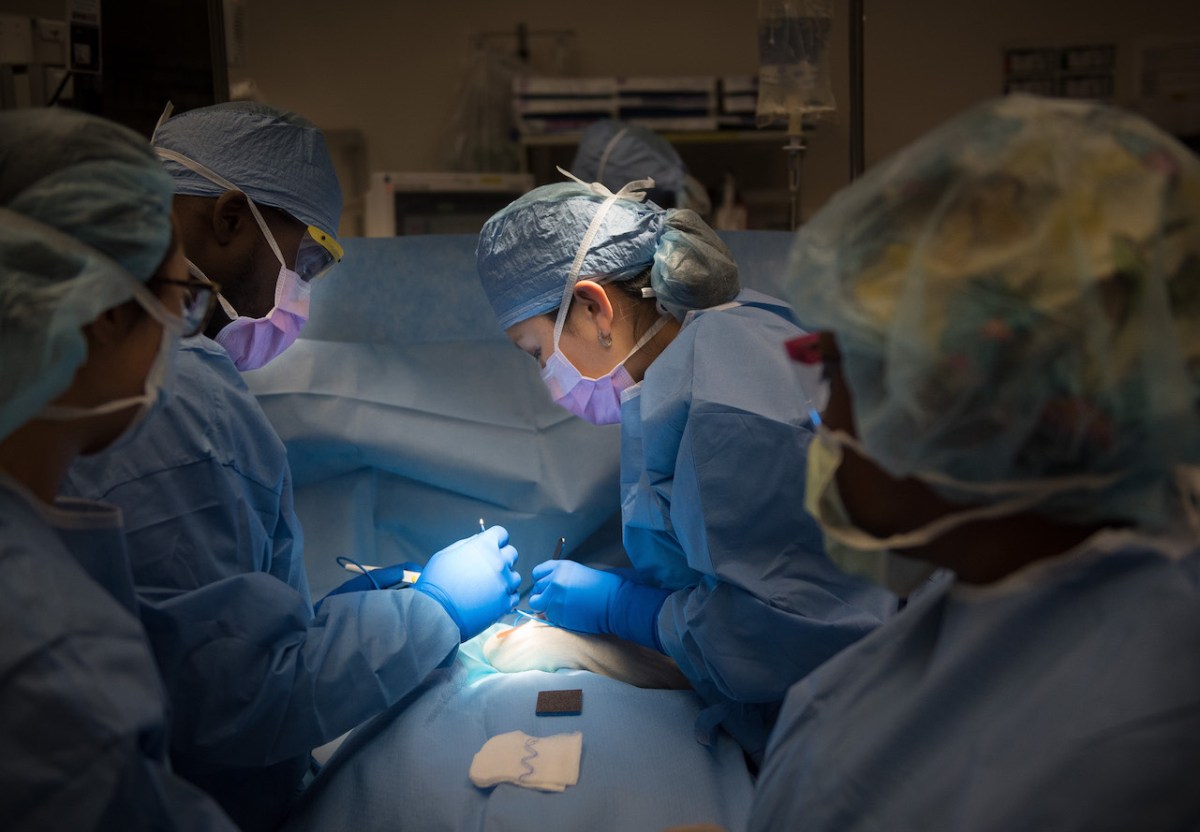
The operating room is the place where I have the privilege of helping children feel better. It’s a very calming place, like a temple. When I walk through the operating room doors, the rest of the world becomes quiet. Even if it is a high-intensity case when the patient is very sick, I know there is a team of nurses, scrub techs and anesthesiologists used to working together in a well-orchestrated fashion. So even when the unexpected arises, we can focus on the patient with full confidence that we’ll find a solution.
There are occasions when babies are so sick that we need silence in the operating room. Everyone becomes hyper-attuned to all the beeps on the monitors. When patients are not as critically sick, I often play a Pandora station that I created called “Happy.” I started it with Pharrell Williams’ “Happy” and then Pandora pulled in other upbeat songs, including a bunch of Taylor Swift songs, so everyone thinks I’m a big Taylor Swift fan.
The OR staff call me by my first name. I believe that if everyone is relaxed and feels like they have an equal say in the procedure, we work better as a well-oiled machine for the benefit of the patient.

Favorite task
Some of the most rewarding times of my day are when I sit down with patients and their families to hear their concerns, to reassure them and to help them understand what to expect — and hopefully to make a scary situation a little less so. As a parent, I realize just how hard it is to entrust one’s child completely in the hands of another. I also like to see patients in the hospital as they’re recovering.
Favorite time
The best part of the day is when I come home. When I open the door into the house, my kids recognize that sound and I hear their little footsteps as they run towards the door, shrieking with joy.
Evening ritual
When my husband and I get home, on nights I am not on call, I cook dinner in the middle of the chaos of hearing about the kids’ day. Hopefully, we “sit down” to eat by 6:20 or 6:30 p.m., and I mean that term loosely. It’s a circus, but eventually everyone is somewhat fed.
And then we do bath time and bedtime. There’s a daily negotiation with my three-year-old on how many books we read before bed. On school nights, she’s allowed three books but she tries to negotiate for 10.
Eventually, we get both kids down for the night. Then my husband and I clean up the mess of the day and try to have a coherent conversation with each other. But by then both of us are exhausted. I try to log on again to finish some work, read or review papers. I usually go to sleep around 11 p.m.
Managing it all
When I can carve out time to do relaxing things for myself, like go to the gym, that is great. But it’s rare and I remind myself that I am blessed with a job that I love and a wonderfully active family.
The result sometimes feels like chaos, but I don’t want to wish my life away waiting for my kids to get older and for life to get easier. Trying to live in the moment, and embracing it, is how I find balance.
Photos by Rachel Baker
This is a reposting of my Scope blog story, courtesy of Stanford School of Medicine.